Liver Detoxification Explained - Part II (+ Complete Protocol)
This article is going to be a long one — over 9,000 words — so take your time with it. Make yourself a cup of tea, maybe even a nice “detox” herbal blend to set the mood, and settle in. I genuinely believe this will be one of the most in-depth and comprehensive pieces you’ll read on the subject of detoxification. I’ve tried to make it thorough, clear, and grounded in real physiology from start to finish. So get comfortable, take a sip, and enjoy the read.
Introduction
On Wednesday, February the 25th, I released a lengthy article about liver detoxification, explaining what it was, the science behind it and the main nutrients involved. I stated that I would do another article, in order to go into further details. It’s time to get to the real things and to actually get this detoxification done. In this post, you will find a detailed protocol, explaining how to do it, which nutrients to use, and so much more.
In the December 2025 issue of the medical journal Nutrients, a very interesting study was published on the impact of modern lifestyles and diet on liver health and the development of new diseases such as non-alcoholic fatty liver disease (NAFLD). This study is very interesting and highlights the complex links between liver health, the gut-brain axis, and oxidative stress.
The study also focuses on the types of food and nutrients most likely to prevent the disease from worsening, thus enabling an effective preventive approach to this modern ailment. For a long time, the medical profession believed that alcohol was the only real risk to liver health. It is true that alcohol is the most toxic and most popular compound that can cause real damage to the liver.
But the study goes much further. Seeing such an article in such a respected journal is extremely encouraging. The article emphasizes the essential role of foods rich in polyphenols, a natural compound found in most fruits and vegetables. Targeting these “functional foods” will play an essential role in managing patients’ conditions to ensure a better quality of life.
The emergence of clinical conditions such as NAFLD demonstrates the negative influence of the modern environment on the liver health of many people. And these are not isolated cases. In France, where I live, we are seeing more and more reports of young people with “fatty liver.” Why is this happening? How can we deal with it? That’s what I’d like to discuss in this article, which will be quite long and comprehensive, but this is a very important topic.
Short Introduction About the Liver
If you haven’t read my first article on liver detoxification that I published the other day, I’ll give you a quick reminder about the role of the liver. If I had to use an analogy, I would say it’s the body’s sorting center, the place where all molecules, food, and vitamins are processed so they can be extracted from the body. However, not all molecules are created equal. The liver is responsible for purifying the body, helping it fight foreign bodies such as toxins, and metabolizing medications and hormones, among other things.
Liver activity can be measured by transaminases (AST and ALT), which are enzymes produced by the liver. Their blood levels are therefore an indicator of liver health. High transaminase levels may be due to liver disease or another health problem. Many medications put pressure on the liver, such as acetaminophen (Tylenol), among many other molecules.
Your liver is one of the most important organs in your body. It filters your blood, processes the nutrients you eat, helps regulate hormones, and breaks down substances that could otherwise harm you. Most of the time, it works quietly in the background without you noticing it. The key to supporting your liver is not extreme detox programs, but simple, consistent habits: balanced nutrition, adequate protein, essential micronutrients, good sleep, and minimizing unnecessary toxins. When you take care of your liver, you support your overall energy, metabolism, and long-term health.
When the liver is not working well, real problems can arise. This is what we will discuss in the article. But first and foremost, we need to understand how we got here. We need to go back to basics and to the time when we were still hunter-gatherers. We will try to understand why we have so many liver problems.
“The greatest medicine of all is teaching people how not to need it.”
— Hippocrates (attributed)
Part 1. A New Chemical Environment
RFK Jr.’s arrival at the head of the Department of Health has raised a lot of eyebrows around the world. But let’s not mock this man. He has some rather controversial theories at times, but he raises a real issue. He arrives and takes on the FDA, which is not necessarily an agency that has worked for your health, let’s put it that way. The problem with “alternative medicine” and the world of wellness is this. When news comes from an agency like the FDA or a government agency, they immediately doubt it and take the opposite view. In the same way, people in “conventional medicine” immediately doubt what comes from naturopaths. The two groups face each other like dogs at a fence, when they potentially have a lot to say to each other.
RFK deserves credit for putting his foot down and unambiguously denouncing the current system, which is directly responsible for the avalanche of chronic diseases in the Western world: junk food.
This is the sad reality that this man is trying to denounce: there is no financial or strategic interest in having healthy people. It is a sad reality. Please note that I am not indulging in conspiracy theories or the kind of behavior that can be found on Facebook forums. I am aware that thimerosal and heavy metals have been present in vaccines for over 20 years. I want to make it clear that my work here will be evidence based, and will always be supported by clear demonstrations.
In 2025, Lazarevic and al. published a comprehensive peer reviewed paper With or Without You? — A Critical Review on Pesticides in Food, which analyzes the growing presence of pesticides in food and their effects on human health. It discusses agricultural practices and addresses the issue of soil depletion, among other issues. Its conclusion is relatively clear: we are heading toward an increase in the presence of pesticides.
Scientific analyses generally show that pesticide residues — including organophosphate, herbicide and other agrochemical compounds — are regularly detected in a range of food crops, depending on agricultural practices and enforcement of maximum residue limits. Chronic dietary exposure is linked in the literature to potential health risks, including endocrine disruption, neurotoxicity, reproductive effects and cancer risk, although regulatory agencies carefully monitor exposure thresholds.
As we will see, some people are more at risk than others. These include people with a variant of the MTHFR gene, linked to folate metabolism, tend have lower glutathione production and find it more difficult to detoxify. This is a real issue, which I will discuss in the article. If you like, you can consult this paper, which explores the subject in depth and will help you understand the links between certain genetic mutations, low antioxidant capacity, and the accumulation of toxins in the body. The topic of the MTHFR gene is very popular nowadays, and should be of special interest for you too. In a 2024 paper, Abozeid (al.) published a peer-reviewed review article discussing how MTHFR is a rate-limiting enzyme in the folate cycle, which provides one-carbon units essential for methionine, S-adenosylmethionine (SAM), and downstream pathways including glutathione synthesis and cellular redox balance.

It explains that common MTHFR polymorphisms (such as C677T and A1298C) reduce enzyme activity, leading to hyperhomocysteinemia, disrupted folate metabolism, and perturbations to pathways linked to oxidative stress and liver pathology such as fibrosis. This study is extremely interesting, as it clearly shows a relationship between a particular genetic SNP and liver disease. As William Walsh so aptly puts it, the link between methylation, oxidative stress, and glutathione is a kind of “Bermuda Triangle” of biochemistry, where many mysterious things happen. If you understand the relationships between homocysteine, methylation, and glutathione production, you will have understood one of the mysteries of health, in my opinion. But that’s what I’m going to help you do in this article.
In this paper, the authors conclude that some genetic SNPs can really put pressure on the liver of people, through the chemical processed exposed above. As you know, biochemical individuality is a very important principle, that should guide your reasoning if you really want to understand your body. The MTHFR gene is simply one example of this.
There is a theory in evolutionary psychiatry that I really enjoy studying, which is the concept of “genome lag.” The idea is simple and helps explain the avalanche of chronic diseases we are experiencing. It is based on the idea that there is a growing gap between the messages we send to our bodies and its ability to interpret these new genetic messages. About 15 years ago, epigenetics was discovered, the idea that our genes are influenced by the signals we send them. In 100 years, our lifestyles have changed considerably, while our biochemical architecture is the same as it was 2,000 years ago (our bodies). Our bodies and nervous systems still live in the age of hunter-gatherers. The tsunami of chronic diseases must be interpreted in light of this growing gap between the messages received by our genome and its inability to process them. Our bodies simply do not understand what is happening, and they struggle as best they can. Toxins, pesticides, drugs, constitue genetic informations that the body tries to decipher, with great difficulty sometimes.
The concept of genome lag is closely linked to evolutionary medicine, particularly through the work of George C. Williams and Randolph Nesse. In their influential book Why We Get Sick, they argue that many modern diseases arise from a mismatch between our ancient genetic adaptations and today’s rapidly changin
g environment. Their work helped establish the idea that understanding evolution is essential to understanding health and disease. This topic is extremely interesting and very useful to analyze our societies.
Our current environment is not the one for which evolution intended us to live. To heal, we must seek to restore this balance and reduce the genome lag, providing the body with the right information so that it can function normally again. The most profound example of the genome lag is the Greek Island of Ikaria, where almost all people live up to 90 years of age.
The genome lag theory can be used to analyze all diseases and all areas of medicine. In psychiatry, we have anxiety and depression; in cardiology, the rise of heart disease. But for the subject that interests us today, the liver, we also have indicative signs. The next section will be devoted to this.
Part 2. The Rise of Non-Alcoholic Fatty Liver Disease (NAFLD)
Metabolic Stress as a Marker of Liver Strain
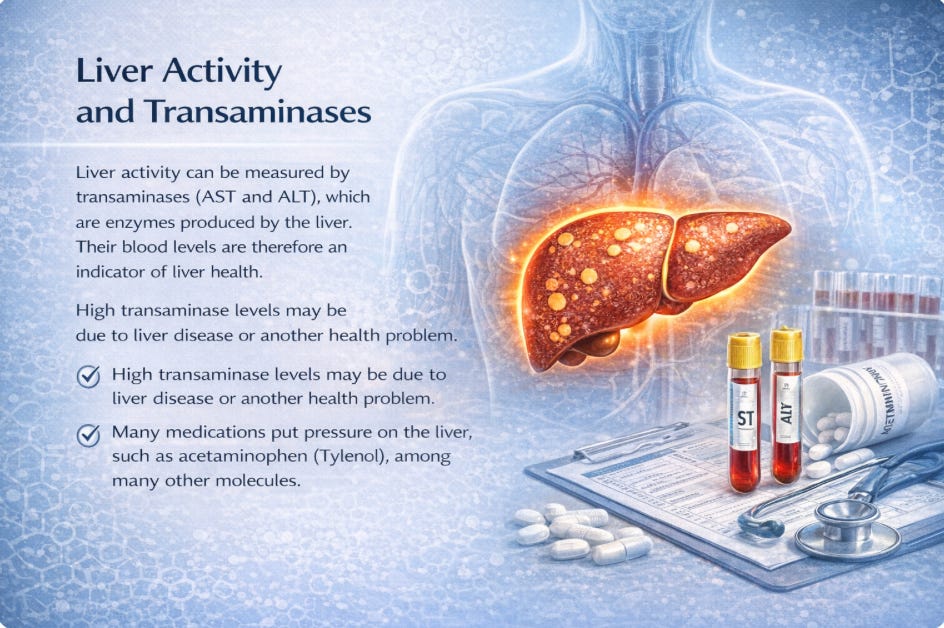
NAFLD is a disease of modern civilization, as well as depression, diabetes, and so on. The thing is that those diseases have a lot in common. They are all related to your metabolism. NAFLD affects approximately 25-30% of the global population. Now the most common liver disorder in industrialized nations, it is strongly associated with obesity, type 2 diabetes and metabolic syndrome. This kind of disease was quite rare before the rise of industrial food system, the addition of pesticides to food. In many ways, this medical condition reflects the evolution of our societies. More and more people are affected and still don’t know it.
From a medical point of view, NAFLD is an accumulation of triglyceride inside hepatocytes. This condition is defined by fat deposition in the absence of significant alcohol intake. For long, the medical profession thought that only alcohol could be responsible for such dramatic liver tissues degradation. The problem with this condition is that it is often silent in the early stages. Like for many metabolic conditions, it is also linked to insulin resistance, a process you may be familiar with. What I find crazy is how little this condition is talked about in the media and even on forums and Facebook groups. I think that this is very important to raise awareness on this issue, as it could help many people.
“Nature does not rush, yet everything is accomplished.”
— Lao Tzu
Part3. From Fat Accumulation to Oxidative Burden
In my opinion, I believe that the pathological process unfolds as follows. The accumulation of triglycerides creates an unfavorable situation, in which mitochondria are severely impacted in terms of energy production and regulation. Insulin resistance creates a very unfavorable situation. This tends to increase ROS generation, leading to oxidative stress.
When faced with oxidative stress, we have more oxidized molecules, which lose an electron and become unstable. We therefore have a greater demand for antioxidants, particularly glutathione, the most important hepatic antioxidant. This point is very important, and I will come back to it later. NAFLD is not only fat accumulating in some parts of the liver, it goes beyond this actually. This is why the use of some nutrients is absolutely essential to recover from it. Fat accumulation creates oxidative burden, which put pressure on nutrient demand of the body.
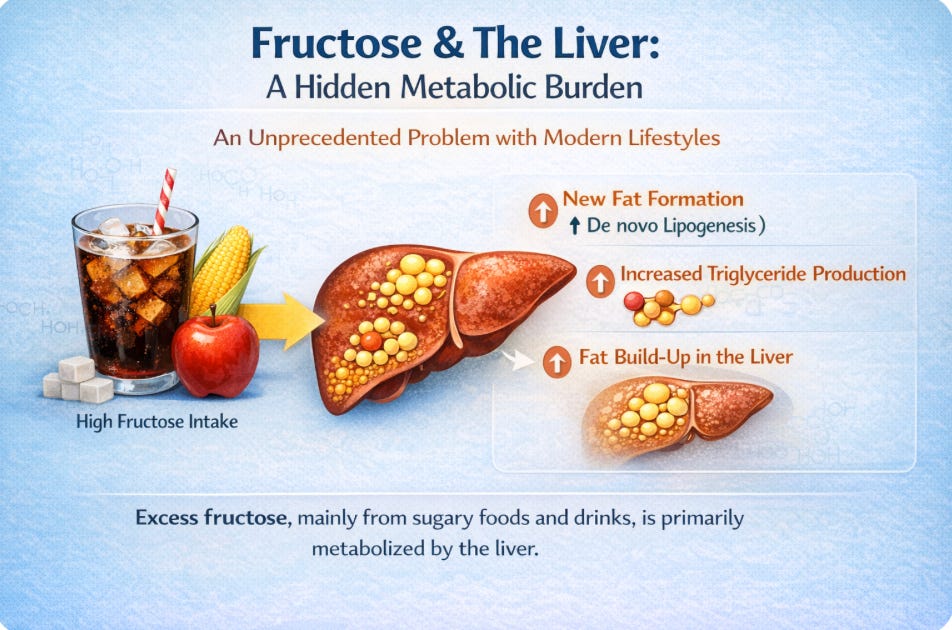
As my friend Kevin Kirkpatrick MSc. has brilliantly demonstrated in his articles on the subject, modern food has a very negative impact on liver health. Some foods are worse than we might have thought, particularly fructose, which can aggravate NAFLD. In this short subsection, I will outline the various “modern drivers” of this disease from a biochemical and molecular perspective.
First of all, there are, of course, ultra-processed foods, which are among the biggest problems. But there are also other interesting factors:
- high fructose intake, present in fruit
- a sedentary lifestyle
- chronic calorie excess (especially carbs)
- lack of sleep
- high cortisol levels
So, in certain specific situations, eating too much fruit is not necessarily good for your health, but this is an exception. All of this will allow you to understand that NAFLD is not merely a fat in the liver. It is a marker of systemic metabolic overload, mitochondrial strain and reduced adaptative bandwidth in modern environment. In the last part of this paper, you will learn how to implement a comprehensive protocol, including the three different phases of liver detoxification. Are you ready for that ?
I would like to point out that what I am doing here is providing a detailed biochemical description of the phenomenon. Just because fructose is involved does not mean you should stop eating fruits. It is important to always take a holistic view. Fruit contains fructose, but it is also very rich in B vitamins, vitamin C, and other nutrients. I know all of this can seem very complicated, but I will make it simple for you. Steps by steps.
I am simply providing a very detailed explanation so that people have all the information they need to decide what they want to do. All the advantages and disadvantages of fructose will be discussed in the final protocol (last part of the article)
Part. 4 Nutrient Deficiency and Oxidative Stress in a Calorie-Rich World
French writer and novelist Georges Bernanos said that “modern life was a conspiracy against all forms of inner life.” I tend to agree with him, but I think he should have added that it was also a conspiracy against health. I think many of my readers will agree with me.
Modern life and modern nutrition present some major problems. Our societies face a great paradox: caloric abundance combined with biochemical insufficiency. It is true that our food has too much calories and not enough nutrients to turn this food into energy.
This phenomenon is what the English physician Derrick Lonsdale brilliantly named high caloric malnutrition. excess carbohydrate intake combined with insufficient micronutrients, particularly thiamine. The body don’t have enough instruments to turn its food into energy, if you like.
Thiamine (vitamin B1) is essential for mitochondrial energy production. As glucose intake rises, thiamine demand increases. When intake fails to match metabolic load, cells experience functional deficiency.
The result is reduced ATP production and increased oxidative stress. For the liver — which must regulate glucose, lipids, redox balance, and detoxification — this mismatch narrows metabolic resilience. What Lonsdale described is precisely the situation our livers are exposed to today. Too much demand and not enough energy to. Too much garbage and not enough cleaner, if you prefer.
Detofixication requires raw materials. Liver detoxification occurs through enzymatic transformation. Phase I reactions activate compounds. Phase II reactions conjugate them, as I explained in my part 1 article. The reactions are not abstract processed, they require:
Amino acids (glycine, cysteine and methionine)
Sulfur containing molecules
B-vitamins (especially B2, B6, B9 and B12)
Zinc
Selenium
Magnesium (for ATP synthesis)
The most important goal of this process is to maintain a stable and steady reserve of glutathione (GSH), so the liver is able to neutralize free-radicals more efficiently. Glutathione is very dependent on cysteine availability, glycine, ATP production and enzymatic cofactors. Methylation is also important, and depends on folate, B12 status. All of this will be included in my protocol. Without adequate of all of those substrates and cofactors, the detoxifications reactions cannot happen in the right way, and your body is struggling. As I said earlier, modern dietary patters rally complicate this reality. Ultra processed food are energy dense but nutrient deficient.
Understanding the Vicious Cycle
If you follow my work, you know that I place particular importance on nutrient deficiencies. While writing this article, I realized something. If we consider that the liver is the organ responsible for detoxifying the entire body, then a deficiency in the liver can have a snowball effect and affect the rest of the body even more. I will try to explain why. Moder life creates a dual constraint, during which micronutrients density is reduced and become less available. At the same time, oxidative stress increase and create a higher demand for nutrients.
nd this is where the vicious cycle begins.
Reduced mitochondrial efficiency leads to:
Lower ATP production
Increased reactive oxygen species
Impaired beta-oxidation
Greater lipid accumulation within hepatocytes
As fat accumulates, oxidative stress increases further.
As oxidative stress increases, glutathione is depleted more rapidly.
As glutathione declines, detoxification and redox buffering become less efficient.
This, in turn, amplifies inflammatory signaling and metabolic dysfunction.
The liver does not suddenly fail. It enters a self-reinforcing loop of strain. The same usually happens in chronic anxiety states, when the body is depleted in nutrients
Fat accumulation increases oxidative stress. Oxidative stress impairs mitochondrial performance. Impaired mitochondria reduce metabolic flexibility.
Reduced flexibility promotes further lipid storage and inflammation. When your metabolism is stuck in a loop, things can go really wrong. If there is a thing to remember, it’s this. If you are reading this sentence, it means that I got your attention to this point, so thanks a lot for reading me.
How to Know if The Detoxification is Working
The term detoxification is often used in a vague and imprecise way, yet it is based on a clear process that can be measured using objective and precise markers. That is the topic I will address in this section.
How do you know if it works?
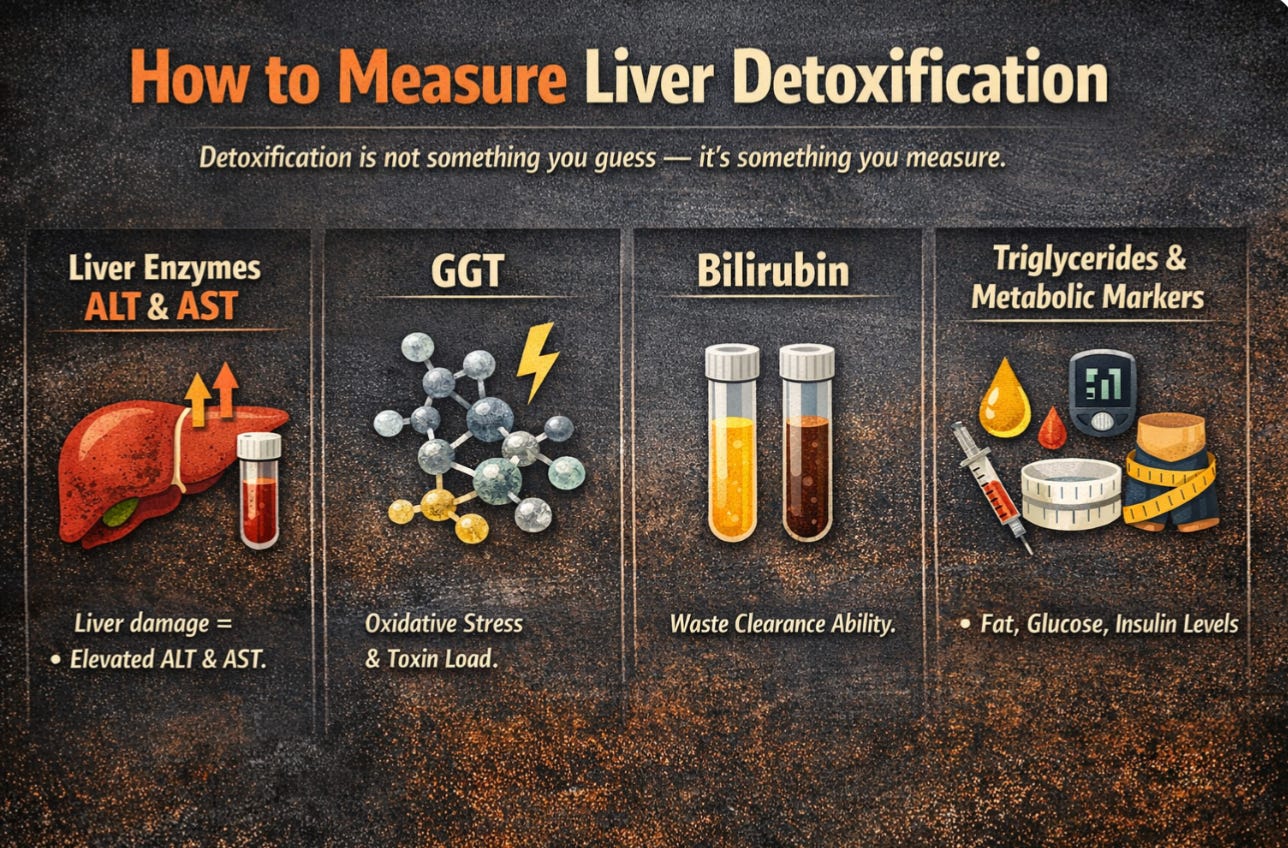
Detoxification is not something you guess — it is something you measure.
1. Liver Enzymes (ALT & AST)
ALT and AST are enzymes found inside liver cells.
When the liver is stressed or damaged, they rise in the blood.
Improvement means elevated levels gradually move toward normal and remain stable over time.
What matters most is the trend, not a single test result.
2. GGT
GGT is closely linked to oxidative stress and glutathione activity.
High levels may reflect liver strain from toxins, alcohol, or metabolic stress.
A decrease in elevated GGT can indicate reduced oxidative burden and improved liver resilience.
3. Bilirubin
Bilirubin reflects the liver’s ability to process and eliminate waste products.
Stable, healthy levels suggest proper detoxification and clearance. This marker is important, especially in the phase II and III of the detoxification process. While you implement the first part of my protocol, it is absolutely useless to asses bilirubin, in my opinion.
4. Triglycerides & Metabolic Markers
Because fatty liver is strongly connected to metabolism, improvements often include:
Lower triglycerides
Better fasting glucose
Improved insulin sensitivity
When metabolism improves, liver function usually follows.
But dear subscribers, I think there is also one factor that should not be underestimated. A good way to know if a therapy is working is if you feel better and your symptoms disappear. Someone with liver problems and brain fog will simply feel better if the protocol works.
This is an important factor! Very important.
Part. 5 Discover the Liver’s Superfoods !!!!
In this section, I will analyze different foods and their respective concentrations of several molecules known to boost liver function. I will divide this into six chemical compounds, focusing on antioxidants such as selenium, glutathione, polyphenols, among others.
I decided to use this format because I think it can be useful for people to have access to examples of specific diets and dishes that can really help the liver function better. I will first give a brief overview of the different food groups, and then suggest two or three dishes.
Glutathione
Sulfur Rich Foods
Sulfur is essential for phase II liver detoxification. Cruciferous vegetables like broccoli, Brussels sprouts, kale, and arugula contain glucosinolates.
These compounds help activate detox enzymes and improve toxin conjugation.
Allium vegetables such as garlic, onions, and leeks provide organosulfur compounds.
Sulfur supports the synthesis of glutathione and other protective molecules.
Regular intake enhances the liver’s natural detox capacity. If your grandmother told you that garlic was very good for health, she was right. Thanks grandma !!
Proteins :
The liver requires adequate protein to repair and regenerate tissue.
Glutathione synthesis depends on amino acids from dietary protein.
Eggs, sardines, salmon, and grass-fed beef provide complete, high-quality protein.
Plant sources like lentils and chickpeas contribute additional amino acids and fiber.
Low protein intake can impair detoxification and antioxidant defenses. This is another reason why the vegan diet is far from being good for health, even if some influencers claim the opposite. The so called soy protein foods are not absorbable like meat, dairy products, eggs and the other foods mentioned here.
A consistent daily intake supports metabolic stability and liver function.
Selenium:
Selenium is required for glutathione peroxidase, a key antioxidant enzyme.
This enzyme protects liver cells from oxidative stress and lipid peroxidation.
Brazil nuts are among the richest natural sources of selenium. Sardines, eggs, and seafood also contribute meaningful amounts. Adequate selenium intake enhances the liver’s defense system. Balanced intake is essential, as both deficiency and excess can be harmful. Selenium is one of the few nutrients that can have a toxic effect if you go above the recommended doses, but anything between 100 to 300mcg is safe for most people.
If you want to learn more about it, I would encourage you to check the book Orthomolecular Medicine for Everyone, published by Abram Hoffer and Andrew Saul in 2008.
Polyphenols:
Polyphenols are plant compounds that reduce oxidative stress and inflammation.
Blueberries and blackberries are rich in anthocyanins with antioxidant properties.
Green tea provides catechins that support metabolic and liver health. Pomegranate contains punicalagins linked to improved antioxidant capacity. Dark cocoa (85%+) delivers flavonoids that protect vascular and hepatic function. Regular intake helps counteract inflammatory stress associated with modern lifestyles. This is the reason you can give to your doctor to claim that wine is actually good for you :) !!!
As a French man, I’m very happy about th
Finally, I will present a diet suitable for people looking to boost their liver function. This diet is quite comprehensive in itself. To maximize its potential, you can add a few supplements included in my protocol. I will give two examples of complete meals, with full nutritional descriptions of the foods.
Meal 1 — Salmon & Cruciferous Support Plate (Lunch)
Main protein source:
Grilled salmon (150–180 g)
Provides high-quality complete protein and omega-3 fatty acids, which help reduce hepatic fat accumulation and inflammatory signaling.
Sulfur-rich vegetables:
Steamed broccoli
Lightly sautéed Brussels sprouts with garlic
These provide glucosinolates and organosulfur compounds that support phase II detoxification pathways and glutathione synthesis.
Polyphenol component:
Fresh arugula salad with pomegranate seeds
Adds additional phytonutrients and antioxidant support.
Trace mineral support:
1–2 Brazil nuts
Provides selenium to support glutathione peroxidase activity.
This meal combines amino acids, sulfur compounds, selenium, omega-3 fatty acids, and polyphenols in a single plate to support multiple detoxification pathways simultaneously.
Meal 2 — Egg, Lentil & Allium Repair Plate (Dinner or Brunch)
Main protein base:
3 eggs
Lentil and chickpea warm salad
Provides complete protein from eggs and additional plant-based amino acids and fiber from legumes to support glutathione production and metabolic stability.
Sulfur-rich vegetables:
Sautéed kale with onions and leeks
Fresh garlic added at the end of cooking
Supports detox enzyme activation and sulfur availability.
Polyphenol beverage:
Green tea
Provides catechins that help reduce oxidative stress and support liver metabolism.
Optional addition:
A small portion of 85% dark cocoa
Adds flavonoid-rich polyphenols that support antioxidant balance.
Part. 6 The Gut-Liver Axis: An Overlooked Relationship
My friend Kevin, that I cited above already, wrote some very interesting paper on the gut liver axis and how both can influence the health of the other. Gut health and probiotics are a big hype since a few years, and for good reasons. After all, digestion is the most important biochemical process in energy production in the body. As I always say, food is basically biochemistry in action. Let’s see.
In 2010, Moschen and al. published a paper attempting to assess the impact of intestinal dysbiosis on the progression of NAFLD, and also analyze other factors involved in the deterioration of liver tissue. They discussed at length the role of microbiota in this process.
As you probably know, our gut is made up of billions of tiny bacteria, probiotics, and prebiotics, which have a major influence on our digestion, mood, and our entire body. Neurotransmitters such as serotonin, dopamine, and other beneficial molecules are converted from food via amino acids (tryptophan, tyrosine, among others). However, small workers are needed to do this job, and if these workers are not healthy, then the work is less effective.
To understand the link between liver health and digestion, we need to look at several processes and concepts, including the barrier between the stomach and the blood.
In normal situations, the barrier remains intact, but in some situations, it can become leaky (the leaky gut). If this happens, some molecules and harmful products will enter the blood stream. As a result, your immune system will respond and try to combat those intruders, through the release of inflammatory molecules like cytokines, like IL-6 (interleukin 6), specific inflammatory mediators released in the gut and in the liver cells via the mast-cells. Those stimulate the secretion of CRP (C-reactive protein) in the liver, which is the main indicator of inflammation in the body.
You also have IL-1β (Interleukin-1 beta), a very potent form of inflammatory mediators which have been proven to influence the progression to NAFLD in several studies. This study right here is very interesting if you want to study the process further. In another paper, the suppression of IL-1β was proven to slow down the progression of NAFLD and NASH, another liver disease. In my protocol, I will focus on some precise inflammatory factors like those, and present studies about some targeted nutrients and foods like garlic, milk thisle, and son on.
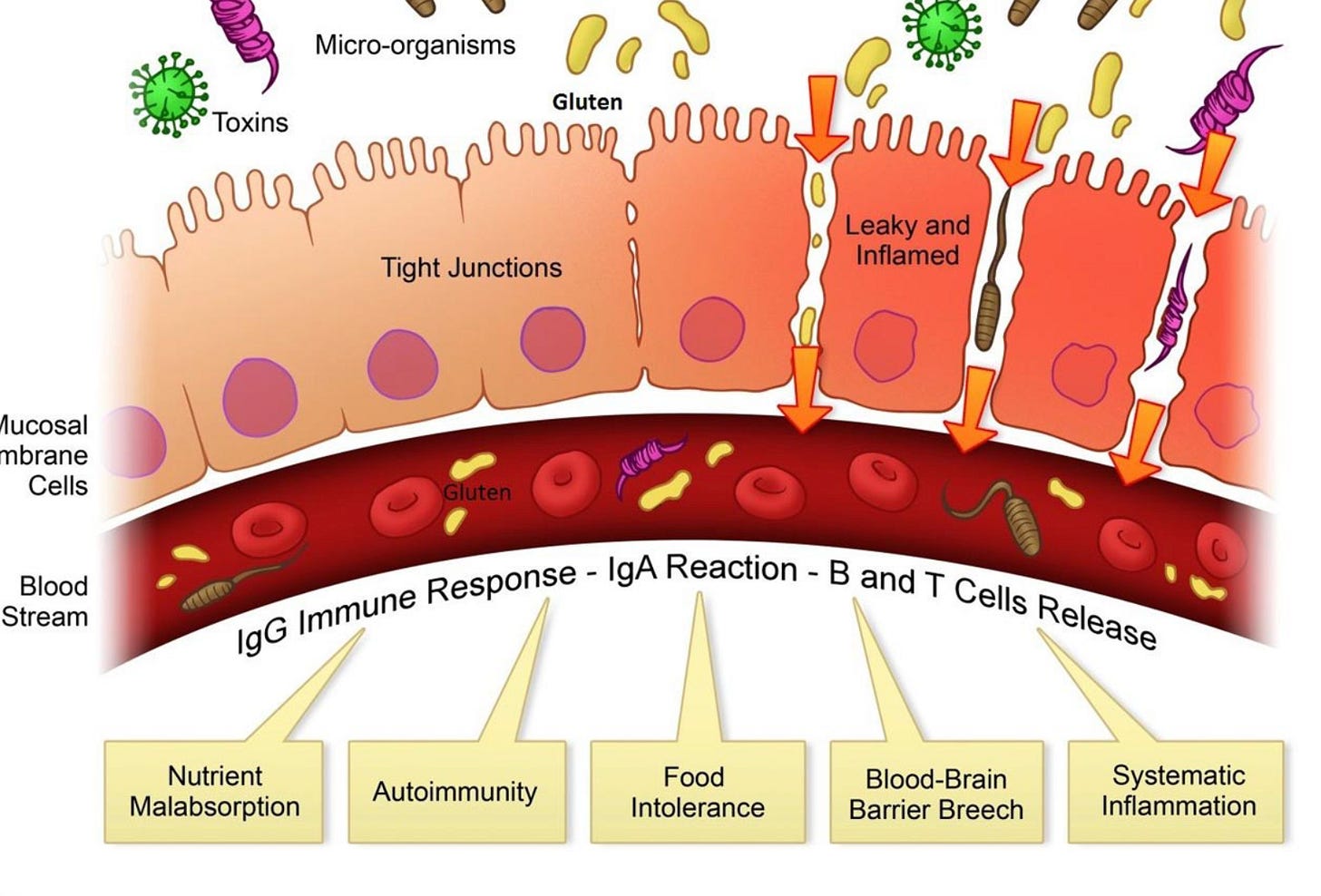
When toxins enters the blood-stream, your immune system is under heavy activation and don’t understand what is going on. Inflammation is like a form of alert signal. If this barrier becomes more permeable (“leaky gut”), small fragments of bacteria — especially a molecule called LPS — can pass into the bloodstream. From there, they travel directly to the liver through the portal vein.
When LPS reaches the liver, it activates immune cells. The liver interprets this as a threat and turns on an inflammatory response. It begins producing inflammatory messengers such as TNF-alpha, IL-6, and IL-1 beta, that I cited above.
These molecules are useful in short-term defense, but when they remain elevated, they create chronic inflammation. Over time, this persistent inflammation can interfere with insulin signaling, increase fat accumulation inside liver cells, and gradually contribute to fatty liver disease. You ned nutrients to fight inflammation, like omega 3s and antioxidants. Ascorbic acid and zinc can both fight inflammation efficiently, and help you resolve this.
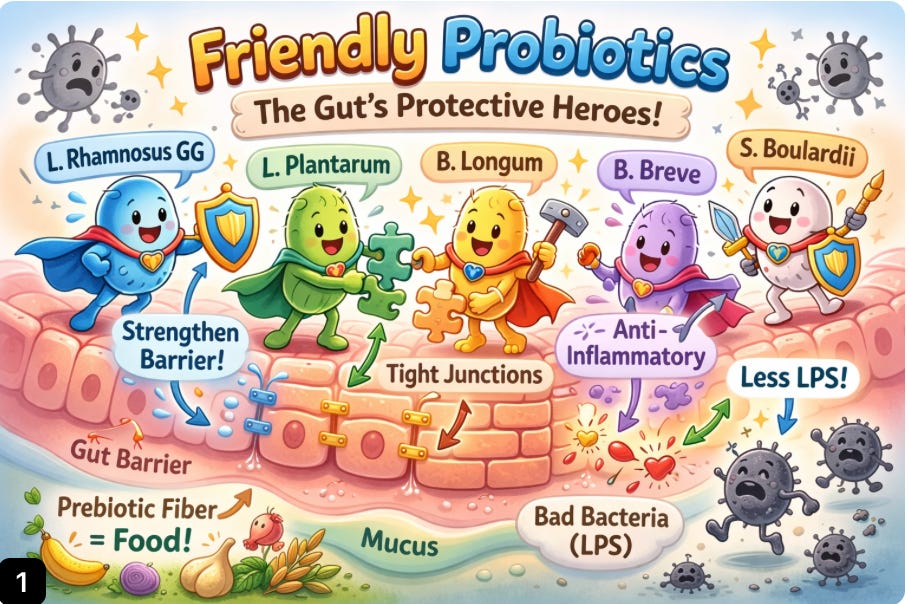
So what, you may ask ? What should I do now with all of those complex informations. Thankfully, there are a lot of steps that you can take to improve or prevent this process. One thing is to take probiotics, molecule that will support your healthy gut bacteria and restore the barrier. It’s hard to find good probiotics and reliable brand, so I made you a list about the most studied and evidence based strains:
Lactobacillus rhamnosus (GG)
Lactobacillus plantarum
Lactobacillus casei
Bifidobacterium longum
Bifidobacterium breve
Bifidobacterium bifidum
Saccharomyces boulardii (levure probiotique)
Lactobacillus acidophilus
Would you ever have thought that a microorganism could protect your life and ultimately save it? You see, life will remain a mystery for a long time to come.
I am going to present a few brands of probiotics that I consider to be reliable. These supplements are often expensive and of poor quality. Studies have shown that more than 8 out of 10 supplements were composed of inactive microbes, despite their high price. Don’t be fooled. I am going to introduce you to two foods known to be the richest in probiotics:
- raw sauerkraut
- kimchi
Finally, I recommend the brand “Natural Factors,” which is one of the highest quality brands I know. It manufactures very good probiotics and is ISURA certified, a label that certifies it is free of more than 700 pollutants.
A recent meta-analysis of randomized clinical trials examined the effects of probiotics in patients with non-alcoholic fatty liver disease (NAFLD). The researchers found that probiotic supplementation was associated with improvements in liver enzymes (such as ALT and AST), better insulin sensitivity, and improved lipid profiles. Some studies also reported reductions in liver fat. While results vary between trials, the overall evidence suggests that supporting the gut microbiota may play a beneficial role in managing NAFLD.
When I first got interested in functional nutrition and health, I was a bit skeptical about all the hype about probiotics and gut health. I honestly thought this was a thing of naturopath, that it was not really serious nor effective. I confess this with a bit of shame today ahah.
When used correctly, probiotics can be a very effective treatment and will not only improve what you are trying to cure. Numerous studies have demonstrated a link between intestinal dysbiosis and diseases such as ALS, Parkinson’s disease, and of course anxiety and depression, among others. I plan to write detailed articles and protocols on the subject at a later date. I invite you to consult the work of my friend Kevin Kirkpatrick MSc. for more information on the subject. He has published several articles on it.
I will not go into further detail about gut health and probiotics, I will write more articles in the future about it. Feel free to do your own research about it, it’s a passionating topic, at least for me. It’s incredible to see that little molecules like this can have such a dramatic impact on health and complex systems of the body.
A Note About Specific Populations : Biochemical Individuality
As I explained above, there are significant differences in people’s biochemistry. I believe that some people are at greater risk of developing liver problems. The main gene is MTHFR, which codes for folate metabolism and tends to greatly reduce glutathione synthesis. I believe that for these individuals, an NAFLD protocol should include bioactive folate (5-MTHF or folic acid). I am specifying this because it will not be included in the protocol that follows.
The most studied gene is PNPLA3 (I148M variant), which promotes fat accumulation in the liver and increases the risk of inflammation and fibrosis. This genetic SNP can really predispose people to develop NAFLD and other liver related problems. In the study enclosed below, you will find many informations about it,.
TM6SF2 (E167K variant) is another important gene that reduces fat export from the liver, leading to triglyceride buildup.
The two last genes that I just cited have a direct link on NAFLD development, via fat accumulation in the tissues. The MTHFR gene has only an indirect link via the reduction of glutathione synthesis in the liver, increased oxidative stress and inflammation. I don’t know how those tests are covered by insurance policies, but I suspect that only hematologists are able to prescribe those. However, you can still contact a private lab testing company like 23andMe and other things. I don’t have any interest or contract with those labs. Make sure that their privacy policies are secure. I heard some mitigated opinions and reviews about 23andMe, even if it’s currently the most populate gene testing service in the US and in the Western World.
You don’t want your genetic data and biological identity to be sold on the dark web. Yes, this happened.
We’ve explored the science — from gut permeability and inflammation to genetics and key nutrients that support liver function.
Now it’s time to move beyond theory.
The liver does not respond to quick fixes or extreme cleanses. It responds to consistent, structured support over time.
In the next section, we shift from understanding to action and present a complete, practical detoxification protocol designed to strengthen liver resilience in a measurable way.
If detoxification is a matter of capacity rather than force, then the logical response is not stimulation — but support. Before attempting to “enhance” elimination, the priority is to reduce metabolic burden and restore biochemical sufficiency. The liver does not need to be pushed; it needs resources, stability, and margin. This is what this protocol will be about.
By rebuilding substrate availability, improving redox balance, and lowering chronic inflammatory load, we widen adaptive bandwidth. The protocol that follows is designed with that principle in mind: restore first, then optimize.
Part. 7 Complete Liver Detoxification Protocol (Three phases)
Now, it is time to get into the real thing and what matters most: how to get this done. In this comprehensive section, I will present a protocol in two divided parts, for each phases of the detoxification process. The protocol here is supposed to be implemented during a five months period. It include three different phases, each one addressing a precise biochemical process.
I’m going to do something unusual, which is to use only articles from PubMed to scientifically support detoxification. Even if detoxification remained confined to naturopathy, but some very interesting papers were beginning to be published on the subject in conventional journals.
In 2023, a very detailed study was published on the subject, comparing the effect of a structured detoxification protocol (phase II) over 28 weeks, similar to what I am proposing here. Two groups were studied, one group simply following a nutritional program (diet) and another group using a diet plus specific supplementation, consisting of several nutrients aimed at stimulating the enzyme glutathione-l-transferase (GSH).
Participants receiving the supplemented regimen showed increases in phase II detoxification enzyme activities, including glutathione-S-transferase. Antioxidant enzymes such as superoxide dismutase were also elevated in this group. The intervention was well tolerated with no major adverse effects reported. These findings suggest that a structured dietary approach may support certain enzymatic pathways of metabolic detoxification, though clinical implications require further research.
PHASE 1 — Foundations (Weeks 1–4)
Reduce Total Metabolic Load
Remove Major Stressors
Eliminate alcohol (temporary full removal preferred)
Remove ultra-processed foods
Eliminate high-fructose beverages
Avoid heating food in plastic
Use filtered water
Reduce Glycemic Volatility
30–40g protein per meal
No refined carbohydrates alone
12-hour overnight fasting window
20–30 minutes daily walking
High fructose intake — especially from sugar-sweetened beverages — directly promotes fatty liver. Because fructose is primarily metabolized in the liver, it strongly stimulates de novo lipogenesis (new fat production). A study in the Journal of Clinical Investigation (Stanhope et al., 2009) showed that fructose-sweetened drinks significantly increase liver fat and cardiometabolic risk. https://pubmed.ncbi.nlm.nih.gov/19381015/
You can also use reduce insulin resistance and hepatic fat accumulation. Practicing intermittent fasting can be a very good and efficient way to restore insulin sensitivity in a majority. However, it should always be used as an add-on measure and not serve as a stand alone tool. I found that IF was very effective in a lot of people, especially people with pre diabetes. This is now supported by some interesting evidence, including very conservative medical journals.
Getting enough protein is absolutely essential. Protein is rich in all amino acids, including tryptophan, glycine, and especially methionine, which will help your body restore effective methylation. This is a very important aspect of the protocol.
Restore Core Nutrient Sufficiency
Detoxification requires substrates. This is why this part will focus on supplying the necessary building block to your whole body. We always heal the body, not an isolated organ, it’s very important to remember this.
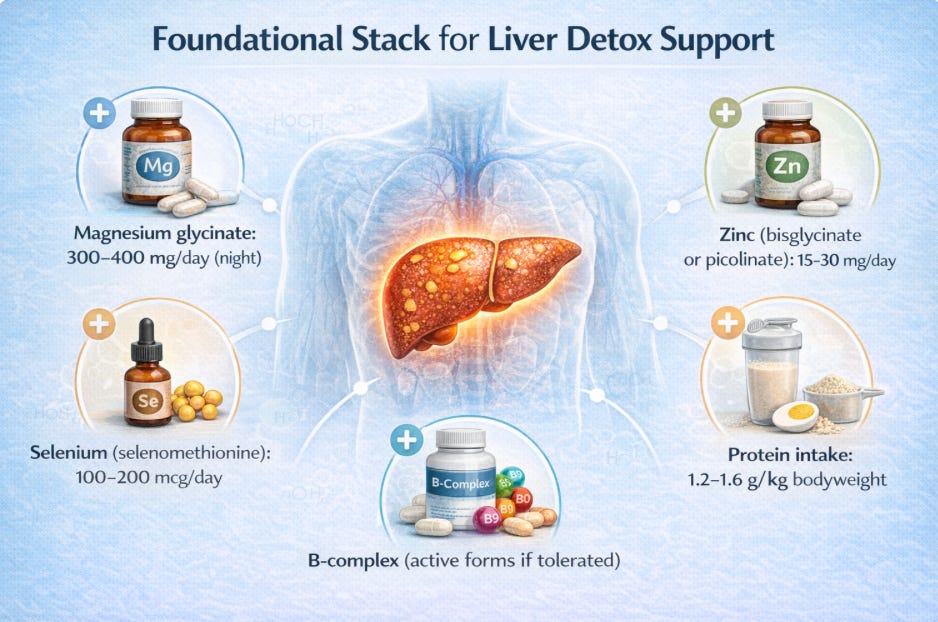
Foundational Stack
Magnesium glycinate: 300–400 mg/day (night)
Zinc (bisglycinate or picolinate): 15–30 mg/day
Selenium (selenomethionine): 100–200 mcg/day
B-complex (active forms if tolerated)
Protein intake: 1.2–1.6 g/kg bodyweight
Optional:
Glycine: 3–5 g at night
Taurine: 1–2 g/day
Goal: restore Phase II conjugation substrates.
The purpose of this section is simple: to provide energy to the body and increase its antioxidant capacity. Selenium and zinc help protect the liver from oxidative stress. B vitamins, combined with magnesium, stimulate ATP production, thereby providing energy to cells, which is essential for restoring liver health. This step is quite simple and does really require further details and explanations. The most important phase, the real detoxification process, is in phase II, in the next part of this article.
Make sure you balance the zinc in a 15:1 ratio with copper, otherwise you could develop copper related anemia, even if it requires a few months of supplementation to reach this point.
PHASE 2 — Glutathione & Redox Restoration (Weeks 4–8)
Only begin if energy and digestion are stable. The goal of this phase is to restore the redox potential of the liver and to restore glutathione reserve. This is the most important phase, where things really happen.
Support Glutathione Production
NAC: 600 mg/day (increase to 600 mg twice daily if tolerated)
Glycine: 3–5 g/day
Vitamin C: 2000 to 4000mg a day
NAC is the direct precursor of glutathione, is very cheap and is very effective for a lot of people. Some studies have shown that it can boost glutathione very quickly and effectively in all people with NAFLD.
Optional advanced:
Liposomal glutathione: 250–500 mg/day
Alpha-lipoic acid: 100–300 mg/day
Alpha lipoic acid (ALA) is useful because it makes other antioxidants in the body more powerful. It recycles vitamin C and glutathione by acting as an electron donor to antioxidants that have lost one, thereby reactivating them. Adding ALA is a very good way to potentiate your other supplements.
You know that I’m a huge believe in the healing powers of vitamin C, so you could perfectly add some liposomal vitamin C to this regimen. You can prefer this form in 1 to 2 grams a day. It is slightly more expensive than regular vitamin C but have the advantage to enter the cells readily.
Improving Mitochondrial Energy
During the first part of this article, I described how fat accumulation and oxidative stress can actually weakens your cells energy supply (mitrochondria). Therefore, one goal of a complete protocol should be to restore ATP synthesis and to maintain healthy energy levels within the cells. In the first phase, I included magnesium glycinate, which is a very good tool to boost ATP levels and to support the whole metabolism of the body.
The enzymes responsible for insulin sensitivity and synthesis are very much dependent on magnesium, among other things. Therefore, this supplement can really have a dual action that will be very beneficial to you.
CoQ10: 100–200 mg/day
Acetyl-L-carnitine: 500–1000 mg/day
Light resistance training 2–3x/week
Goal: restore ATP production and reduce ROS generation. CoQ10 is especially valuable if you are more than 35 years old. After this age, the synthesis of this molecule is lowered and you can really be deficient in it. If you have been suffering from liver problems and fatigue, it is very likely that you will improve on it. Please find enclosed two sources about this very topic:
A randomized, double-blind, placebo-controlled clinical trial investigated the effects of Coenzyme Q10 (100 mg/day) in patients with non-alcoholic fatty liver disease (NAFLD). After four weeks of supplementation, participants receiving CoQ10 showed a significant reduction in AST levels—a key liver enzyme marker—along with improvements in certain metabolic parameters compared to placebo. These findings suggest that CoQ10 may help support liver function in individuals with fatty liver, although longer-term studies are needed to confirm sustained benefits.
PHASE 3 — Phase II & Bile Support (Weeks 8–12)
Only introduce when inflammation is lower and digestion stable. This process should be implemented when you recovered most of your energy and when you just feel better overall.
Increase Cruciferous Vegetables
Broccoli sprouts
Arugula
Brussels sprouts
Cabbage
Optional:
Standardized sulforaphane extract
Supports Nrf2 activation and detox gene expression. Sulforaphane is present in veggies and especially in things like Brussels Sprouts and things like that. Rhonda Patrick did some very interesting things on this. You will find many resources on Youtube.
Gentle Hepatic & Biliary Support
Milk thistle (silymarin 150–300 mg/day)
Artichoke extract
Dandelion root tea
Goal: support hepatocyte resilience and bile flow — not force elimination. This is a very important part of the protocol too. Milk Thistle has been evaluated by many researchers for its myriad of benefits and has a very low potential of toxicity.
Hajaghamohammadi et al., Randomized Clinical Trial – Silymarin in NASH
In this randomized controlled trial, patients with non-alcoholic steatohepatitis (NASH) received 210 mg/day of silymarin for 8 weeks. The study reported significant reductions in AST and ALT levels compared with placebo, suggesting an improvement in biochemical markers of liver function.
PHASE 4 — Long-Term Metabolic Optimization
Address NAFLD Risk Factors
Reduce visceral fat (aka, lose weight)
Increase muscle mass
Improve sleep (7–8 hours)
Limit fructose intake
Lifestyle Variables (Often More Important Than Supplements)
Daily movement
Consistent sleep schedule
Stress regulation (breathing, sunlight exposure, resistance training)
Avoid chronic caloric surplus
This protocol may not work for everyone but it constitutes a very structured and comprehensive example of a liver detoxification protocol. You can add other things, like probiotics and a lifestyle protocol too (exercise, etc). But I’m quite happy about it.
Before closing, I want to leave you with something simple. This protocol — and your health in general — does not need to be perfect to work. You don’t have to apply everything flawlessly or control every variable. The liver does not respond to extremes; it responds to steady support over time. If you move in the right direction most days — better food choices, more protein, fewer obvious stressors, consistent nutrients, better sleep — that is already enough to create change. What matters is the trend, not a single meal or a single missed supplement. Sustainable progress will always beat short bursts of perfection followed by burnout. Because in severe cases of liver detox, things can go worse before they got better.
When all the toxins are flushed out of the body, things can go worse and you may think that your symptoms worsen, when in fact it’s a sign that it’s working. I’ve seen many cases of severe heavy metal poisoning and of scared people that stopped the protocol because their blood values of heavy metals were increasing. But this is a sign that this is working. When the liver is working fully again, it will help the body to excrete poisons from the tissues, and then will flush them out via the blood stream. This is a very important point.
Stay consistent, stay patient, and trust that your body knows how to recover when you give it the right conditions. I don’t want you to live like Brian Johnson and to be the ultimate human. Just be yourself.
This article was pretty long to write but it was worth it I think. Liver health is such an important topic and I feel like more people would benefit from it.
I decided to create a protocol based on clear scientific evidence that is understandable to all readers. The protocol can be followed using only 5 to 6 nutrients for both phases. It is important to always consider the body as a whole and not focus solely on the liver as an isolated organ in the center of the body.
Today, many people suffer from NAFLD without even knowing it. So I am very happy to have been able to write an article and send it to my 3,600 subscribers. I know that I have about 1,000 regular readers, or 30% of my audience, which is very good for such a specific niche as nutrition. As William Walsh said, even if you do this work to help just one person, it will have been worth it. I agree. Like some of the founding fathers of functional medicine and naturopathy, I believe that liver detoxification can have a positive impact on many diseases, including the most serious ones.
By restoring liver function, the entire body environment is transformed for the better.
Figures such as Max Gerson, Jeffrey Bland, and Linus Pauling recommended this procedure, saying that it would allow the body to restore its normal metabolism. Because metabolism is energy. And energy is life.
I will conclude my remarks with these words and thank you from the bottom of my heart for reading.
References:
Lazarević-Pašti, T., Milanković, V., Tasić, T., Petrović, S., & Leskovac, A. (2025). With or Without You?—A Critical Review on Pesticides in Food. Foods, 14(7), 1128. https://doi.org/10.3390/foods14071128 — Article: https://www.mdpi.com/2304-8158/14/7/1128
Abozeid, F. (2024). Associations of methylene tetrahydrofolate reductase (MTHFR) polymorphisms with liver-related outcomes. Egyptian Liver Journal. https://link.springer.com/article/10.1186/s43066-024-00342-7
Nesse, R. M., & Williams, G. C. (1994). Why We Get Sick: The New Science of Darwinian Medicine. Times Books. https://books.google.com/books/about/Why_We_Get_Sick.html?id=9lhxDKuRn1QC
Bland, J. S. (2014). The Disease Delusion: Conquering the Causes of Chronic Illness for a Healthier, Longer, and Happier Life. HarperOne. https://www.goodreads.com/book/show/18505814-the-disease-delusion
Tilg, H., & Moschen, A. R. (2010). Evolution of inflammation in nonalcoholic fatty liver disease. Hepatology, 52(5), 1836–1846. https://pubmed.ncbi.nlm.nih.gov/21038418/
Wang, Q., Wang, X., Pang, J., Zheng, Y., Cao, J., Feng, J., Ma, Y., & Wei, Y. (2022). Probiotics for the improvement of metabolic profiles in patients with MAFLD/NAFLD: Meta-analysis of randomized controlled trials. Frontiers in Endocrinology. https://pubmed.ncbi.nlm.nih.gov/36407321/
Kazeminasab, F., et al. (2024). The effects of probiotic supplementation and exercise training on NAFLD: Systematic review and meta-analysis of RCTs. https://pubmed.ncbi.nlm.nih.gov/39090657/
Panda, C., et al. (2023). Guided Metabolic Detoxification Program Supports Phase II Detoxification Enzymes and Antioxidant Balance in Healthy Participants. https://pubmed.ncbi.nlm.nih.gov/37432335/ — Full text: https://pmc.ncbi.nlm.nih.gov/articles/PMC10181083/
Stanhope, K. L., et al. (2009). Consuming fructose-sweetened, not glucose-sweetened, beverages increases visceral adiposity and lipids and decreases insulin sensitivity in overweight/obese humans. The Journal of Clinical Investigation, 119(5), 1322–1334. https://doi.org/10.1172/JCI37385 — PubMed: https://pubmed.ncbi.nlm.nih.gov/19381015/
Farsi, F., et al. (2016). Functions of Coenzyme Q10 Supplementation on Liver Enzymes and Metabolic Markers in NAFLD: A randomized, double-blind, placebo-controlled trial. https://pubmed.ncbi.nlm.nih.gov/26156412/
Solhi, H., et al. (2014). Silymarin in treatment of non-alcoholic steatohepatitis: A randomized clinical trial.https://pmc.ncbi.nlm.nih.gov/articles/PMC3894463/
Hajaghamohammadi, A., et al. (2008). The Efficacy of Silymarin in Decreasing Transaminase Activities in Non-Alcoholic Fatty Liver Disease: A Randomized Controlled Clinical Trial. https://brieflands.com/journals/hepatmon/articles/70029
Hoffer, A., & Saul, A. W. (2008). Orthomolecular Medicine for Everyone: Megavitamin Therapeutics for Families and Physicians. https://books.google.com/books/about/Orthomolecular_Medicine_for_Everyone.html?id=mUIrfIcsX1IC
Walsh, W. J. (2012). Nutrient Power: Heal Your Biochemistry and Heal Your Brain.https://www.goodreads.com/book/show/14603192-nutrient-power
Rinella, M. E., et al. (2023). AASLD Practice Guidance on the clinical assessment and management of nonalcoholic fatty liver disease. Hepatology, 77(5), 1797–1835. https://pubmed.ncbi.nlm.nih.gov/36727674/
Tacke, F., et al. (2024). EASL–EASD–EASO Clinical Practice Guidelines on the management of metabolic dysfunction-associated steatotic liver disease (MASLD). Journal of Hepatology. https://www.journal-of-hepatology.eu/article/S0168-8278(24)00329-5/fulltext
Kozlitina, J., et al. (2024). Global Epidemiological Impact of PNPLA3 I148M on Liver Disease.https://pmc.ncbi.nlm.nih.gov/articles/PMC11815610/
Yan, L., et al. (2023). Therapeutic potential of sulforaphane in liver diseases: A review.https://pmc.ncbi.nlm.nih.gov/articles/PMC10495681/
Li, S., et al. (2024). Administration of silymarin in NAFLD/NASH: A systematic review.https://pubmed.ncbi.nlm.nih.gov/38579127/